TL;DR:
- Effective chronic pain management combines movement, mental health support, lifestyle changes, and therapy.
- Non-drug approaches like exercise, CBT, stress management, and sleep hygiene are the first-line treatments.
- Personalizing strategies based on individual needs and focusing on improving function rather than just pain relief is essential.
Chronic pain touches nearly 25% of US adults, quietly reshaping daily routines, sleep, and mood in ways most people never expected. Many assume that managing it means taking more medication or simply enduring it. Neither is true. Research consistently shows that the most effective strategies combine movement, mental health support, lifestyle changes, and targeted therapies. This article walks you through what chronic pain really is, what the evidence says about managing it well, and how to build a practical plan that fits your life starting today.
Table of Contents
- Understanding chronic pain: What it is and why it persists
- Proven approaches: The pillars of chronic pain management
- Personalizing your plan: Integrating wellness and addressing unique needs
- Risks, myths, and realities: Making informed decisions about chronic pain management
- Taking action: Applying chronic pain management strategies in daily life
- Why chronic pain management is about more than just pain relief
- Discover wellness tools to support your pain management journey
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Chronic pain is complex | It affects millions and requires individualized, ongoing management, not just a quick fix. |
| Non-drug strategies work | Exercise, stress reduction, and healthy habits are proven first-line approaches. |
| Personalized care matters | The most effective pain management matches your unique needs, lifestyle, and health conditions. |
| Know the risks | Opioids and invasive procedures carry significant risks and are not first-line treatments. |
| Practical action improves life | Consistency with self-care, goal setting, and expert guidance leads to improved function and quality of life. |
Understanding chronic pain: What it is and why it persists
Chronic pain is not just pain that lingers. It is a condition in its own right, defined as pain lasting three months or longer, often continuing well beyond the original injury or illness. Understanding why it persists is the first step toward managing it effectively.
There are three main types of chronic pain:
- Nociceptive pain comes from tissue damage, like arthritis or a muscle injury. It is the most familiar type and often feels like aching or throbbing.
- Neuropathic pain results from nerve damage or dysfunction. It often feels like burning, shooting, or electric sensations and is common in conditions like diabetic neuropathy.
- Nociplastic pain occurs when the nervous system itself becomes overly sensitive, even without clear tissue or nerve damage. Fibromyalgia is a well-known example.
For adults between 40 and 65, the most common sources of chronic pain include osteoarthritis, lower back pain, neck pain, and peripheral neuropathy. These conditions often develop gradually, which is part of why they can feel so hard to pin down.
The impact goes far beyond physical discomfort. Chronic pain disrupts sleep, which worsens fatigue and mood. It limits physical activity, which leads to muscle weakness and weight gain. That is the domino effect of physical strain in action. It also raises the risk of depression and anxiety, creating a cycle that feeds itself. In fact, high-impact chronic pain causes major activity limitation in about 8% of US adults.
“Chronic pain is not a symptom to be treated in isolation. It is a condition that reshapes how the body and mind communicate, requiring a whole-person response.”
Supporting your wellness at home is not a luxury when you live with chronic pain. It is a foundational part of managing it well. The more you understand your pain type and its triggers, the better positioned you are to take meaningful action.
Proven approaches: The pillars of chronic pain management
The good news is that effective pain management does not start with a prescription pad. Current guidelines recommend non-drug therapies first and advise against routine opioid use due to risk and lack of long-term benefit. That is a significant shift from how pain was managed even a decade ago.
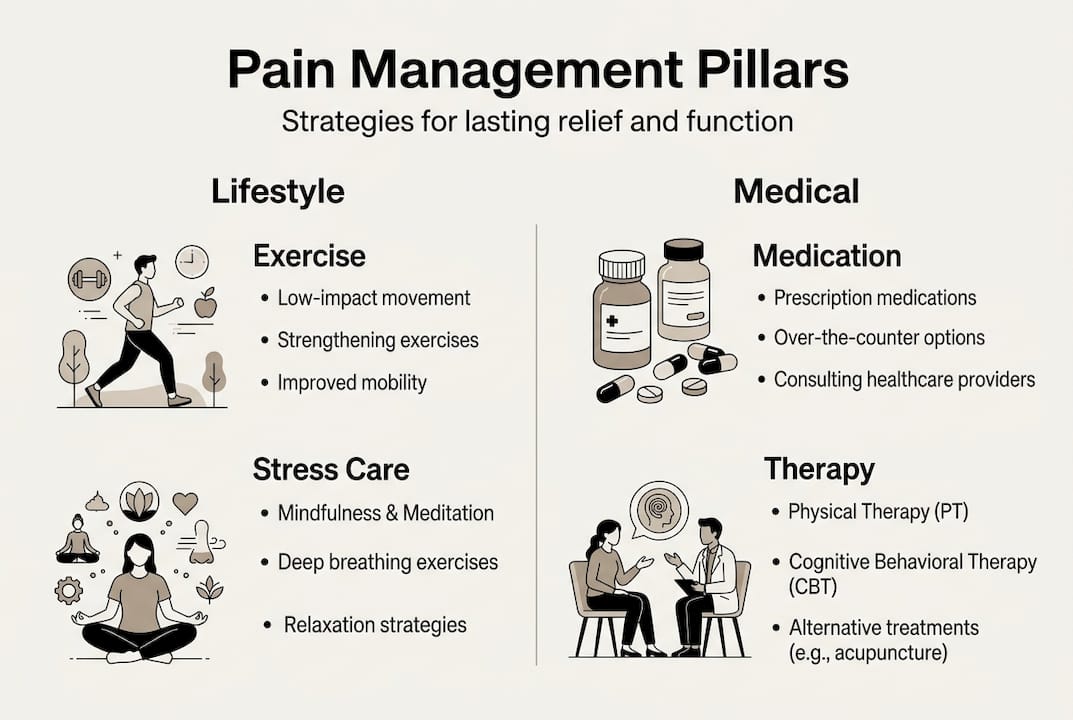
Here are the core evidence-based pillars:
- Exercise and movement therapy. Regular, low-impact movement reduces pain sensitivity and builds strength. Walking, swimming, yoga, and tai chi are all well-supported options.
- Cognitive behavioral therapy (CBT). CBT helps you identify and reframe thought patterns that amplify pain. It is one of the most researched non-drug treatments available.
- Stress management. Chronic stress raises inflammation and pain sensitivity. Breathing exercises, mindfulness, and relaxation techniques make a measurable difference.
- Sleep hygiene. Poor sleep worsens pain perception. Consistent sleep schedules, limiting screens before bed, and a cool, dark room all support better rest.
- Anti-inflammatory nutrition. What you eat influences how much inflammation your body carries. Exploring nutrition for pain management is a practical, low-risk step with real upside.
Multimodal non-pharmacologic strategies reduce pain by 20 to 30% and improve function, making them a strong first-line choice.

| Approach | Evidence level | Best for |
|---|---|---|
| Exercise therapy | High | Arthritis, back pain, fibromyalgia |
| CBT | High | All chronic pain types |
| Anti-inflammatory diet | Moderate | Inflammatory pain, arthritis |
| Opioid therapy | Low (long-term) | Short-term acute flares only |
| Epidural injections | Low-moderate | Specific nerve compression |
When medications are needed, options like tricyclic antidepressants (TCAs), serotonin-norepinephrine reuptake inhibitors (SNRIs), and gabapentinoids can help, especially for neuropathic pain. These are not pain medications in the traditional sense but they work on the nervous system in ways that reduce pain signals. For expert pain care, always work with a provider who understands your full health picture.
Pro Tip: Combining two or more non-drug strategies consistently outperforms any single treatment. Think of your plan as a toolkit, not a single fix. You can explore pain relief strategies that are tailored for active adults to build that toolkit.
Personalizing your plan: Integrating wellness and addressing unique needs
No two people experience chronic pain the same way. Person-centered care and shared decision-making are essential because assessing function matters more than chasing a single pain score. Your goals, your lifestyle, and your health history all shape what works best for you.
Here is what personalization looks like in practice:
- Arthritis: Gentle range-of-motion exercises, warm water therapy, and ergonomic adjustments at home reduce joint strain without aggravating inflammation.
- Fibromyalgia: Sleep hygiene and stress reduction are especially powerful. Consistent routines calm the nervous system over time.
- Lower back pain: Core strengthening, posture awareness, and stress relief work together. Tension in the back is often tied to emotional stress as much as physical strain.
- Neuropathy: Nerve-focused therapies, blood sugar management (for diabetic neuropathy), and gentle movement all help reduce burning and tingling sensations.
Addressing mental health is not optional in this process. Depression and anxiety are present in a significant portion of adults living with chronic pain, and they make pain harder to manage. Wellness strategies including exercise, diet, sleep, and stress reduction improve daily quality of life for adults 40 to 65, and that includes emotional wellbeing.
A solid stress management guide can help you build the mental and emotional side of your plan. Pair it with practical self-care tips and well-being tips designed for your age group.
Pro Tip: Track your pain in relation to sleep, stress, and activity levels for two weeks. Patterns often emerge that reveal your most powerful personal triggers, and that information is gold when working with your care team.
Risks, myths, and realities: Making informed decisions about chronic pain management
Some of the most common beliefs about chronic pain management are simply not supported by evidence. Clearing these up helps you make smarter choices.
Common myths worth questioning:
- “More tests mean better care.” Imaging and diagnostic tests rarely change the treatment plan for common chronic pain conditions. They are most useful when there are red flags like sudden weakness or unexplained weight loss.
- “Chronic pain always needs medication.” Non-drug therapies are first-line for most pain types and carry far fewer risks.
- “If it still hurts, you need a stronger treatment.” Intensity of treatment does not equal effectiveness. Gentle, consistent strategies often outperform aggressive ones.
- “Surgery will fix it.” Surgery is appropriate in specific, well-defined cases but is rarely a solution for widespread chronic pain.
Epidural and joint injections have low-certainty evidence of benefit and notable risks, and most guidelines recommend against routine use. They may have a role in specific situations, but they are not a reliable long-term solution.
| Intervention | Typical benefit | Key risk |
|---|---|---|
| Opioids (long-term) | Modest, short-lived | Dependence, overdose |
| Epidural injections | Variable, often temporary | Infection, nerve damage |
| Surgery (non-specific) | Inconsistent | Complications, recovery |
| Exercise therapy | Consistent, cumulative | Minimal if guided |
Opioid therapy carries significant misuse, dependency, and overdose risks, and most people should avoid long-term use for chronic conditions.
“Asking your provider ‘what is the evidence for this?’ is not being difficult. It is being a smart patient.”
If you are exploring relief without medication, you have more options than most people realize. From natural pain relief options to targeted arthritis pain remedies, evidence-based alternatives are both accessible and effective.
Taking action: Applying chronic pain management strategies in daily life
Knowing what works is only half the equation. The other half is actually doing it, consistently, even on the harder days. Here is how to build a daily plan that holds up in real life.
- Start with one anchor habit. Pick one strategy, like a 20-minute walk or a 10-minute breathing practice, and do it daily for two weeks before adding more.
- Set SMART goals. Specific, Measurable, Achievable, Relevant, and Time-bound goals keep you focused. “I will walk for 15 minutes after dinner, five days a week” beats “I will exercise more.”
- Track your progress. A simple journal or app noting pain levels, sleep quality, mood, and activity gives you real data to work with and helps you spot what is helping.
- Plan for setbacks. Bad days happen. Having a short, gentle fallback routine, like stretching in bed or a warm bath, keeps you in the habit even when energy is low.
- Know when to escalate. If your pain suddenly worsens, spreads, or is accompanied by new symptoms, see your provider. Self-management is powerful but not a substitute for medical evaluation.
Multimodal, holistic management yields real improvements in function and quality of life, especially when strategies are applied consistently over time.
Building on proven strategies and paying attention to posture and comfort throughout your day are two habits that quietly compound over weeks and months.
Pro Tip: Schedule your wellness habits the same way you schedule appointments. Treating them as non-negotiable time blocks dramatically improves follow-through.
Why chronic pain management is about more than just pain relief
Here is something most pain management conversations miss: the goal should never be a lower number on a pain scale. It should be a fuller life.
When you focus only on reducing pain intensity, you can end up chasing treatments that promise quick results but deliver little lasting change. When you shift the focus to what you want to do, whether that is gardening, playing with grandchildren, sleeping through the night, or simply feeling more like yourself, the whole approach changes. You start choosing strategies that build function, not just suppress sensation.
At Lunix, we believe that empowering daily wellness is the foundation of real pain management. The research backs this up. Adults who measure success by what they can do, rather than how much they hurt, tend to stay more motivated, stick with their routines longer, and report better overall wellbeing. That is not a small thing. That is the whole point.
Discover wellness tools to support your pain management journey
Putting a multimodal pain management plan into practice is much easier when you have the right tools supporting you at home. Recovery products designed for daily comfort can fill the gap between clinical appointments and real life.

At Lunix, we design smart recovery tools that fit naturally into your daily routine, whether you need support during rest, movement, or sleep. From ergonomic comfort solutions to targeted recovery products, our wellness solutions are built with adults 40 to 65 in mind. Explore what is available and find the pieces that complement your personalized pain management plan. Your comfort and quality of life are worth investing in.
Frequently asked questions
What are the most effective chronic pain management strategies?
Non-pharmacologic strategies are endorsed as first-line, including exercise, CBT, stress management, and sleep hygiene, with personalized medication added only when needed. Combining multiple approaches consistently delivers the strongest results.
Are opioids recommended for chronic pain management?
Routine opioid use is discouraged by current guidelines for chronic pain due to serious risks of dependence and limited long-term benefit. Short-term, carefully monitored use may be appropriate in specific situations.
Can diet and lifestyle really help manage chronic pain?
Yes. Lifestyle and wellness interventions can improve function and reduce chronic pain symptoms, particularly when healthy eating, regular movement, quality sleep, and stress reduction are combined.
Why do some people need different types of pain management?
Neuropathic and nociplastic pain require different approaches and central-acting therapies compared to nociceptive pain, so individualized care based on pain type and personal health history is essential for best results.
How long does it typically take to find the right pain management plan?
It can take weeks or months of trial and adjustment to discover the best combination of strategies for each person’s needs, and that is completely normal. Patience and consistency are part of the process.




